- Were cycles consistent (15–20 minutes)?
- Did total exposure exceed your protocol limit?
- Was the client uncomfortable mid-cycle (early stop needed)?
Troubleshooting Professional Teeth Whitening Results
Troubleshooting Professional Teeth Whitening Results
Uneven shade change, chalky white spots, gum irritation, or sensitivity spikes after whitening? These are usually protocol issues, not “bad gel”. Use this guide to diagnose the cause fast and fix it without guesswork.
Fast triage: what happened?
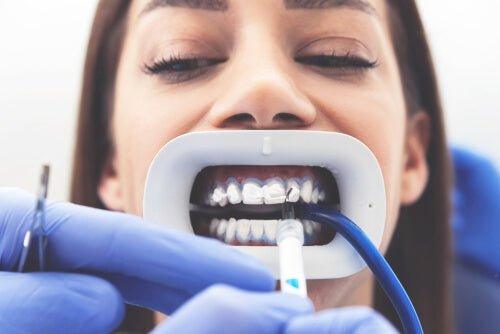
Before you change strength or blame the light, run this 60-second checklist. Most “problems” are one of three things: moisture contamination, soft-tissue exposure, or case selection.
- Was the field truly dry, or did saliva creep in?
- Was gingival barrier fully cured and sealed?
- Any gel pooling at the gingival margin?
- Restorations (crowns, veneers, composite) do not change shade
- Intrinsic stains may require multiple visits
- Client diet and aftercare can sabotage results fast
1) Uneven whitening or banding
Typical look: patchy shade, darker edges, lighter centers, or a “band” near the gumline.
- Uneven gel thickness (too thick in one area, too thin in another)
- Moisture contamination or saliva creep
- Inconsistent light distance/angle (if using light)
- Skipping the prep polish on heavy plaque/stain
- Re-isolate and re-apply a thin, even layer
- Correct lamp positioning (consistent distance across arch)
- If plaque/stain present, polish first then treat
- Consider stepping down strength for sensitive clients and adding another visit
- Use a repeatable application pattern (same order every time)
- Dry field is non-negotiable (retract, isolate, re-check)
- Use the strength ladder instead of overcooking one visit
2) Dehydration lines (chalky look right after)
Typical look: temporary white streaks or a “dry” chalky appearance immediately post-treatment.
- Surface dehydration from isolation and prolonged exposure
- Often looks worse immediately after the session
- Usually normalizes as teeth rehydrate
- Do not re-treat the same day
- Allow 12–24 hours rehydration before judging final shade
- Use gentle aftercare and avoid airflow directly on teeth
- Don’t overdry with air
- Stick to consistent cycle timing
- Guide clients to proper aftercare (48-hour plan)
3) White spots look “worse” after whitening
Typical look: existing decalcification/white spots become more visible right after treatment.
- Dehydration makes contrasts appear stronger
- White spots were already present, but the surrounding shade changed
- Post-whitening rehydration can soften appearance over time
- Wait 24–72 hours before re-evaluating
- Use gentle remineralizing aftercare if appropriate
- Document baseline so clients don’t “discover” it later and blame you
- Explain beforehand: whitening changes contrast, it doesn’t erase defects
- Offer a step-down plan with multiple visits instead of over-strength
4) Gum irritation, burning, or whitening of tissue
Typical look: tender gums, redness, or temporary blanching where gel touched tissue.
- Barrier not fully cured or missing coverage at the margins
- Gel overflow/pooling at gingival margin
- Client movement during treatment causing contact
- Rinse thoroughly and remove all residual gel
- Keep diet gentle for 24 hours (avoid acidic/spicy)
- Update your barrier placement and curing time protocol
- Use a professional gingival barrier and cure fully
- Apply gel thin and controlled (no pooling)
- Re-check margins before each cycle
5) Sensitivity (“zingers”) after whitening
Typical look: short sharp pain triggered by cold air/drinks after the session.
- Peroxide diffusion temporarily increases sensitivity in some clients
- Higher concentrations + longer exposure increase risk
- Back-to-back sessions compound the issue
- Reduce strength next session (use the ladder)
- Space treatments (commonly 7+ days when sensitivity is high)
- Use post-care desensitizing support and strict aftercare
6) “No results” or minimal shade change
Typical look: client expects a dramatic change, sees little or none.
- Intrinsic stains that need multiple visits
- Expired/incorrectly stored gel (heat exposure)
- Heavy plaque/stain not removed before whitening
- Client expectation mismatch (restorations won’t change)
- Confirm gel freshness and storage
- Polish prep for heavy stain cases
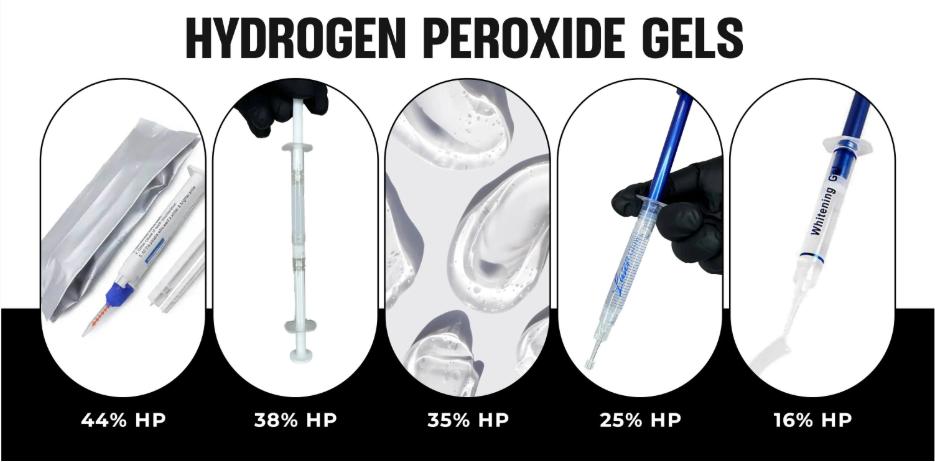
- Use a progressive plan (25% → 35–44% based on case)
- Set a 2-visit plan for intrinsic discoloration
- Don’t brute force one visit. Build outcomes with the protocol ladder.
- Use the hub to select strength properly.
7) Rebound or “it faded fast”
Typical look: client looks great right after, then feels it “dropped” days later.
- Rehydration changes perceived shade after dehydration phase
- High pigment exposure in the first 48 hours
- No maintenance plan
- Reinforce 48-hour white diet
- Offer controlled maintenance options between visits
- Set expectations: the “final look” stabilizes after rehydration
- Give a written aftercare plan (use this)
- Book a touch-up cadence (3–6 months depending on pigment)
- Document starting shade so “memory whitening” doesn’t win
Professional resources that make results predictable
If you want fewer “my teeth look weird” messages, your team needs a consistent system. Start with the hub and use the strength ladder for case selection.
FAQ: troubleshooting whitening issues
Why do teeth look chalky right after whitening?
That’s typically dehydration. It can exaggerate contrasts and make the surface look chalky. Let teeth rehydrate for 12–24 hours before judging final shade.
How long do dehydration lines last?
Often 24 hours. Some cases may take longer depending on isolation intensity and client hydration.
Why are results uneven after whitening?
Most commonly uneven gel thickness, moisture contamination, or inconsistent lamp distance if using light. Fix your isolation and application pattern first.
Do white spots get worse after whitening?
They can appear more visible temporarily due to dehydration and contrast changes. Re-evaluate after 24–72 hours and document baseline before treatment.
Why did gums turn white after treatment?
Temporary blanching can occur where peroxide contacts tissue. It typically resolves within hours. Improve barrier coverage and prevent gel pooling.
How do I prevent gum irritation?
Use a properly placed and fully cured gingival barrier, apply gel thinly, avoid overflow, and re-check margins before each cycle.
What causes “zingers” after whitening?
Temporary sensitivity from peroxide diffusion. Higher strength and longer exposure raise the likelihood. Use a strength ladder and avoid back-to-back high-strength sessions.
How long does sensitivity last after whitening?
Commonly hours to a couple of days. If it persists or worsens, reassess strength, exposure, and client sensitivity history.
Why did whitening not work at all?
Often intrinsic stains needing multiple visits, expired or heat-exposed gel, heavy plaque/stain not removed first, or unrealistic expectations (restorations don’t whiten).
Can crowns/veneers/bonding whiten?
No. Only natural enamel changes shade. Cosmetic planning may be needed after whitening to match restorations.
Should I increase strength if results are low?
Not automatically. First fix isolation and application. Then use the strength ladder based on sensitivity and stain load.
How soon can I re-treat after a session?
Depends on sensitivity and case type. For sensitive clients, spacing sessions (often 7+ days) is common. Avoid re-treating during dehydration.
Why did results fade quickly?
Rehydration changes perceived shade and pigments can re-stain early. Enforce the 48-hour white diet and build a maintenance plan.
Is light required for whitening results?
No. Light can support workflow, but your core drivers are isolation, gel placement, and protocol timing.
What’s the best way to standardize results across staff?
Use a written protocol: same prep, same isolation checklist, same application pattern, and consistent cycle timing. Document each session.
What’s the most common provider mistake?
Moisture contamination. A tiny amount of saliva defeats your oxidation efficiency and creates uneven outcomes.
What’s the simplest “fix” when results are inconsistent?
Slow down and tighten execution: isolation, even application, consistent timing. Strength is not a substitute for discipline.
Where should I learn gel selection and protocols?
Start in the Professional Resource Center and use the Gel Strength Hub for case selection.
Clinically reviewed by David Hanna, RDH. This page is educational and intended for professionals. Always apply appropriate clinical judgment and follow local regulations and scope of practice.